The Polybalm® Study

 The full design of the Polybalm® study can be seen on the official trials website. Polybalm® is the only natural remedy to be scientifically designed, prepared and evaluated in a major government back UK randomized controlled trial (RCT). This summary was taken from the study protocol and the presentation at the American Society for clinical Oncology Conference 2017.
The full design of the Polybalm® study can be seen on the official trials website. Polybalm® is the only natural remedy to be scientifically designed, prepared and evaluated in a major government back UK randomized controlled trial (RCT). This summary was taken from the study protocol and the presentation at the American Society for clinical Oncology Conference 2017.
Read full peer reviewed scientific paper – May 2018
Background
 Nails are made by living stem cells and, because they are dividing rapidly, are especially susceptible to chemotherapy1. As a consequence, disfiguring nail damage is common, especially following regimens containing taxanes used for men and women with breast and prostate cancer. The type and severity of damage is variable, but most intravenous regimens can cause ridges in nails, which correspond to the timings of chemotherapy episodes known as ‘Beau’s lines’. More pronounced chemotherapy nail damage leads to discolouration, brittle nails, acute paronychia, onycholysis and sometimes even complete loss of the nail. This damage is often unsightly and contributes to body image issues during chemotherapy2. More serious consequences include pain, which can limit activities of daily living, and secondary infection. This is of particular concern when patients are also neutropenic as the nails could be a source of systemic infection.
Nails are made by living stem cells and, because they are dividing rapidly, are especially susceptible to chemotherapy1. As a consequence, disfiguring nail damage is common, especially following regimens containing taxanes used for men and women with breast and prostate cancer. The type and severity of damage is variable, but most intravenous regimens can cause ridges in nails, which correspond to the timings of chemotherapy episodes known as ‘Beau’s lines’. More pronounced chemotherapy nail damage leads to discolouration, brittle nails, acute paronychia, onycholysis and sometimes even complete loss of the nail. This damage is often unsightly and contributes to body image issues during chemotherapy2. More serious consequences include pain, which can limit activities of daily living, and secondary infection. This is of particular concern when patients are also neutropenic as the nails could be a source of systemic infection.
In addition to the killing of rapidly proliferating nail stem cells, damage is also thought to be due to chemotherapy’s anti-angiogenetic and neurogenically mediated inflammatory properties5,6,7. If marked, the nails can separate from the bed causing pain, secondary bacterial and fungal infections considerably increasing damage to the nail5,6,7.
A variety of anecdotal strategies are advised to patients during chemotherapy including nail hygiene, wearing nail varnish and avoiding trauma. We have previously published a report showing that cooling the nails bed with pots of iced water helps to reduce its severity4. Understandably, the practice has never caught on within the confines of a busy chemotherapy unit. Commercially available cooling gloves are available but they are not particularly popular among UK chemotherapy nurses as they may cover the veins of the hands and prevent assessment of the patient’s extremities8,9.
Many patient advocacy groups advise massaging moisturising balms into the nail bed, based on assumptions that oiling skin around the cuticles could improve compliance, thus preventing splitting which can be a route for infection and damage the nail bed. Although this seems intuitively beneficial there are no studies to support this practice or advise which balms to use. Patients are also often advised to wear nail varnish despite the knowledge that nail polish removers dry the nails. Likewise, there were no previously published prospective trials to support this practice during chemotherapy, or in an otherwise healthy population.
Development of the investigational balm (Polybalm®)
 The chose of essential oils and waxes were made following an extensive scientific review of the laboratory and clinic data, by the clinical trial trials scientific committee. Following a review of several hundred potential candidates the four oils and four bases were selected not only for their individual properties but that they worked in synergy with each other to ensure their health advantages were complementary and exploited to the full.
The chose of essential oils and waxes were made following an extensive scientific review of the laboratory and clinic data, by the clinical trial trials scientific committee. Following a review of several hundred potential candidates the four oils and four bases were selected not only for their individual properties but that they worked in synergy with each other to ensure their health advantages were complementary and exploited to the full.
The committee itself was unique in that, for the first time, it brought together traditional medical scientist, experienced oncologists and nurses with natural complementary therapist, qualified herbalists and nurses from around the UK all working together with patients themselves. This team then collaborated closely with the National Lifestyle and Behavioural change work stream of the, Department of Health backed, National Cancer Research Network, advisors from the Department of Biological Science at Coventry University and ethics committees from Bedford and Cambridge University Hospital trusts.
Once the ingredients were selected, meticulous care was given to ensuring the correct types and quantities of oils to ensure they could not irritate the skin. The bases contained cold pressed extra virgin olive oil, organic beeswax, unrefined cocoa butter and unrefined organic shea butter. The essential oils included Gaultheria procumbens, lavandula officinalis, eucalyptus globulus, tarchonanthus camphoratus – the full scientific summary of their properties can be viewed on the formal trials website
How these oils prevent chemotherapy induced nail damage:
The waxes and oils in Polybalm® are particularly rich in phytochemical especially the phenolic polyphenols group. In addition to they basic abilities to mosturizing the skin and prevent drying, splitting or cracking of the nail, they are known to have anti-inflammatory and anti-oxidant properties1,2,3. It was hypothesized for the Polybalm® trial that oils with these properties, applied locally to the nail bed, would be sufficient absorption to act as a local antidote to the chemotherapy, preventing damage to the proliferating stem cells. In addition their anti-microbial properties would help prevent secondary infection so overall keeping the nail healthy and intact1,2,3.
Authenticity and quality control of the study:
Investigational balm was manufactured specifically for this study by Power Health Ltd and European product cosmetic tests and certification were performed by Advantis Laboratories Ltd. They fully comply with European Union Cosmetics Standards (product license 76/768/EEC). The trials committee collaborated closely with the National Lifestyle and Behavioural change work stream of the, Department of Health backed, National Cancer Research Network. The committee included independent advisors from the Department of Biological science at Coventry University, it was governed by the Cambridge University ethics committee and registered with the NHS Health Research Authority and all results were analysed by independent statisticians to ensure the best possible, robust and authenticated design.
Trial Design
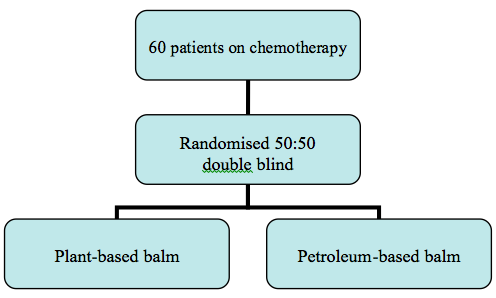 Sixty one men and women receiving chemotherapy for breast or prostate cancer at one of Cambridge University’s affiliated Hospitals (Bedford) over a 2 year recruitment period. After written informed consent, they were randomised (50:50) to apply either a simple petroleum based moisturising balm to their nail bed three times a day or the investigational balm now known as Polybalm®, named after the trial.
Sixty one men and women receiving chemotherapy for breast or prostate cancer at one of Cambridge University’s affiliated Hospitals (Bedford) over a 2 year recruitment period. After written informed consent, they were randomised (50:50) to apply either a simple petroleum based moisturising balm to their nail bed three times a day or the investigational balm now known as Polybalm®, named after the trial.
Trial outcomes measurements: The health of the nails were measured by 4 independent tools and none of the patients, doctors, research team or statistician knew which balm was assigned to which participant.
Patients recorded their own nail health with the validated Dermatology Life Quality questionnaire (DLQQ) plus a simple linear severity scale (LSS) that emphasised how the nail damage affected their daily activities and quality of life.
Physicians recorded the physical condition of the nails using the validated Nail Psoriasis Index (NPSI) plus another simple linear severity scale (LSS). As well as directly scoring nail damage, photographs of the nails were sent to 3 doctors from other departments and hospitals for further independent verification.
Results:
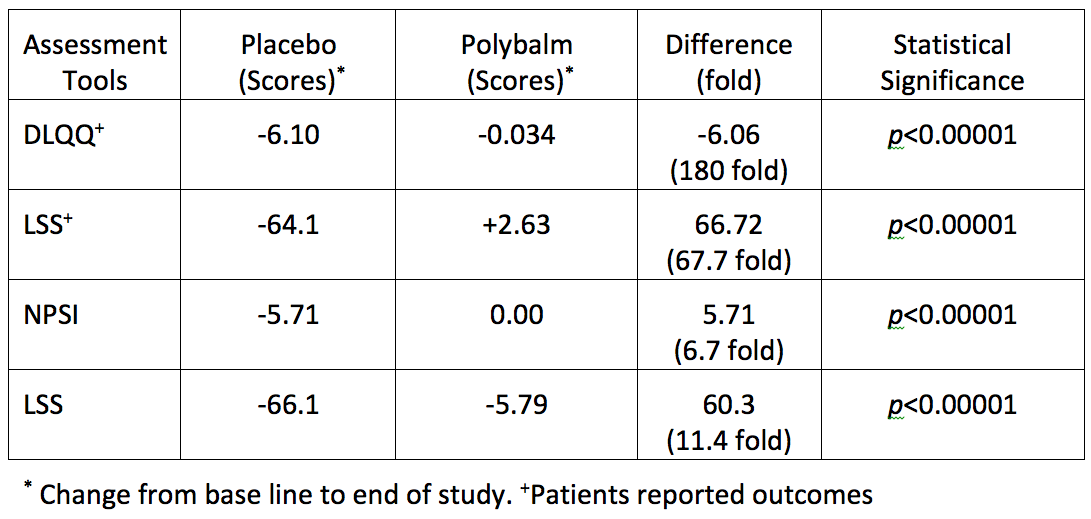 In all but 1 of the 30 patients in the Polybalm® cohort, there was virtually no nail damage compared to more than half suffering significant damage and distress in the placebo group. In fact the average patient reported nail related quality hardly changed in the Polybalm® group and the linear scale actually improved between the start and end of the chemotherapy. There were no reported allerges or adverse events related to either creams. The patients in the Polybalm® group who still had some nail changes also suffered from other severe chemotherapy complications including neutropenic sepsis, diarrhea and peripheral neuropathy. The more complete data is reported in the adjacent table
In all but 1 of the 30 patients in the Polybalm® cohort, there was virtually no nail damage compared to more than half suffering significant damage and distress in the placebo group. In fact the average patient reported nail related quality hardly changed in the Polybalm® group and the linear scale actually improved between the start and end of the chemotherapy. There were no reported allerges or adverse events related to either creams. The patients in the Polybalm® group who still had some nail changes also suffered from other severe chemotherapy complications including neutropenic sepsis, diarrhea and peripheral neuropathy. The more complete data is reported in the adjacent table
Conclusion: The polyphenol rich essential oils and plant-based waxes in this nail bed balm profoundly reduced chemotherapy related nail damage and improved nail related quality of life compared to a plain petroleum based balm. The 180 fold improvement in nail related quality of life will be welcomed by patients suffering this unwelcome toxicity which would otherwise significantly effect up to half of people receiving chemotherapy. The precise mode of action of this investigational balm would require further evaluation to elucidate and it would be interesting to investigate whether combination with nail bed cooling could further reduce the risk of this distressing toxicity in all patients.
